Home › Blog › Fascia and Flexibility
Fascia and Flexibility: Why Stretching Is More Complex Than You Think
Most people treat flexibility as a muscle problem. It isn't. A practitioner-level look at fascial tissue mechanics, nervous system science, and why professional stretch therapy produces results self-stretching simply cannot match.
In This Article
Flexibility Is Not Just a Muscle Problem
Ask most people why they are not flexible and they will tell you their muscles are tight. Ask most fitness professionals the same question and you will get a more nuanced answer — but still one that is often incomplete. The conventional model of flexibility centers on muscle length: stretch the muscle, lengthen the tissue, gain range of motion. If it were that simple, consistent self-stretching would produce consistent, lasting results. For most people, it does not.
The reason is that fascia and flexibility are inseparable — and the fascial system, along with the nervous system that governs it, is far more complex than the muscle-length model accounts for. Understanding this complexity is what separates a practitioner who produces real, lasting mobility improvements from one who is simply applying technique without a mechanism.
This article is written for fitness professionals, stretch therapists, and curious clients who want to understand what is actually happening beneath the surface when professional stretch therapy works — and why it works in ways that self-directed stretching cannot replicate.
What Is Fascia?
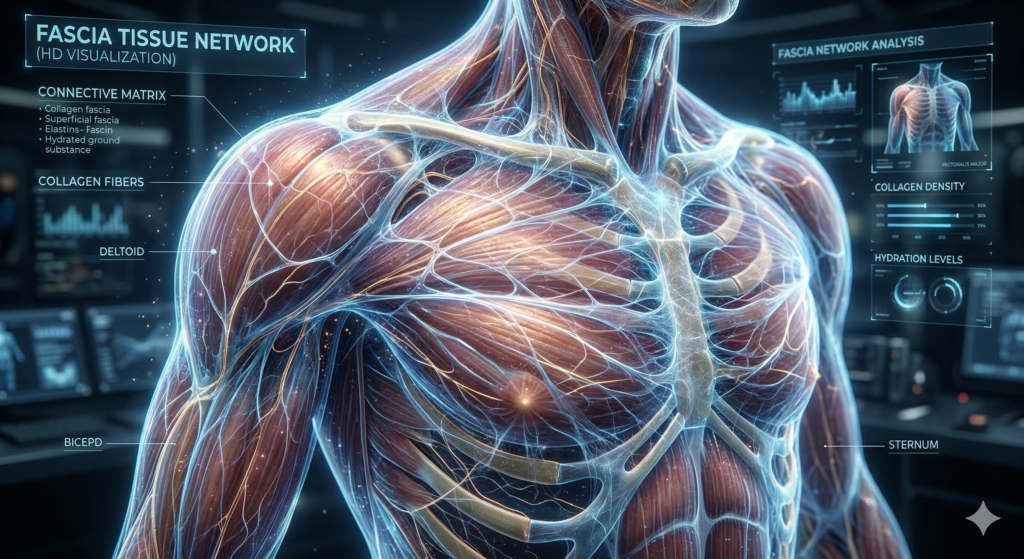
Fascia is the continuous, three-dimensional web of connective tissue that surrounds, separates, and interpenetrates every structure in the human body — muscles, bones, organs, nerves, and blood vessels. It is not passive packaging. It is a highly dynamic, metabolically active tissue with its own sensory capacity, its own contribution to force transmission, and its own role in how the body perceives and coordinates movement.
Fascia is a body-wide connective tissue matrix — composed primarily of collagen fibers, elastin, and a fluid ground substance — that organizes the body into functional units, transmits mechanical force across movement chains, and communicates sensory information to the nervous system in real time.
For most of the twentieth century, fascia was treated as an inconvenient obstacle in anatomical dissection — the white material you cut through to get to the muscles and organs that were considered important. That view has been fundamentally overturned. Researchers now understand that fascia contains more sensory nerve endings than the muscles it encases. It responds to mechanical loading, hydration, movement, and temperature. It adapts — and it maladapts.
When fascia is well-hydrated, regularly moved through full ranges of motion, and appropriately loaded, it maintains a supple, gliding quality that supports free, effortless movement. When it is chronically compressed by sedentary posture, repetitively stressed in one direction, or dehydrated through inadequate recovery, it develops adhesions — areas where layers of fascia that should slide freely against each other become stuck. These adhesions restrict movement, generate pain, and alter how force is transmitted through the body in ways that compound over time.
"The body is not a collection of separate muscles and bones. It is a continuous tensional network — and the fascial web is what gives that network its coherence, its communication, and its capacity for coordinated movement."
Reflected in the work of Thomas Myers, Anatomy TrainsThomas Myers, whose work in Anatomy Trains mapped the body's fascial continuities with unprecedented precision, demonstrated that fascia does not simply wrap individual muscles in isolation. It connects them — in organized, functional pathways that run head to toe, front to back, and diagonally through the body. A restriction anywhere in one of these pathways creates consequences far from its origin point. This insight — that the body is a tensional network rather than a collection of independent parts — is foundational to understanding why fascia and flexibility are so deeply linked.
Fascial Lines and Why Restrictions Travel
One of the most clinically significant discoveries in modern fascia research is that fascial tissue does not operate in isolated segments. It runs in continuous fascial lines — organized chains of connected tissue that link distant parts of the body into functional movement units. Researchers and practitioners in the field have mapped these lines with increasing precision, identifying how specific pathways govern common movement patterns and where restrictions in one region predictably create problems in another.
Superficial Back Line
Runs from the plantar fascia at the sole of the foot, up the back of the legs and spine, over the skull to the forehead. Restrictions here — tight calves, hamstrings, or thoracolumbar fascia — are often experienced as lower back pain or limited forward flexion.
Superficial Front Line
Connects the top of the foot, up the front of the legs and abdomen, to the neck and skull. Tightness in the hip flexors, rectus abdominis, or anterior neck contributes to the postural forward-lean and rounded-shoulder patterns most desk workers develop over time.
Lateral Line
Runs along each side of the body from the foot to the skull, coordinating lateral balance and stabilization. Restrictions here often present as IT band tightness, lateral hip pain, or lateral neck tension — all connected through the same continuous fascial pathway.
Spiral Line
Wraps around the body in a helix, linking the skull, ribcage, pelvis, and feet in a rotational pattern. Restrictions in the spiral line contribute to rotational asymmetry, scoliotic tendencies, and the knee and foot problems that emerge from an imbalanced rotational base.
The clinical implication of fascial lines is significant: a restriction you feel in your lower back may be originating in your hamstrings, your calves, or even the plantar fascia of your foot. Stretching only the area of pain — the conventional approach — addresses the symptom while leaving the source intact. A practitioner trained in fascial anatomy assesses the entire line, not just the complaint site, and addresses the restriction at its origin rather than its expression.
Practitioners at CNU Stretch are trained in the AIS (Alignment Imbalance and Solution) assessment system — a structured framework for identifying which fascial lines are restricted and tracing restrictions to their source. This is why a well-designed stretch therapy session often addresses areas that feel distant from the client's primary complaint — and why those sessions produce results that self-stretching, which targets symptoms rather than sources, cannot replicate.
The Nervous System: The Real Gatekeeper of Flexibility
Fascia is one half of the equation. The other half — and in many ways the more important half — is the nervous system. Flexibility is not primarily a tissue property. It is a nervous system permission.
Your brain is continuously monitoring the state of your body through a network of sensory receptors embedded throughout your muscles, tendons, and — critically — your fascia. These receptors report on tissue tension, joint position, load, and rate of change in real time. Based on this information, your nervous system makes constant decisions about how much range of motion to allow and when to engage protective contraction.
The stretch reflex — the involuntary muscular contraction that fires when a muscle is lengthened too quickly — is the most familiar expression of this system. It exists to protect joints from exceeding structurally safe ranges. But in many people, this protective system is chronically over-tuned. The nervous system fires defensively at ranges of motion that are not actually dangerous, effectively limiting flexibility far below its structural potential.
This is why you can feel "tight" immediately after waking up even though no structural change occurred in your tissue overnight — your nervous system is simply in a higher protective state. It is also why people sometimes experience a dramatic increase in range of motion during a professional stretch session that seems to exceed what the tissue could physically account for. The tissue did not change in those minutes. The nervous system's tolerance did.
Proprioception and the Fascial Sensory Network
Fascia contains a dense network of proprioceptive receptors — Ruffini endings, Pacinian corpuscles, interstitial receptors — that continuously feed positional and mechanical information to the nervous system. This is why fascial health directly affects body awareness, coordination, and movement quality, not just flexibility.
Autogenic Inhibition
When a muscle is held under sustained tension, Golgi tendon organs signal the nervous system to reduce muscular contraction — allowing the tissue to relax into greater length. Professional stretch therapists use timing and positioning to leverage this mechanism, accessing depths of range that the client cannot reach through self-directed effort alone.
Neuromuscular Re-Education
With consistent, methodical practice, the nervous system learns to tolerate greater ranges of motion without triggering defensive contraction. This process — neuromuscular re-education — is why the flexibility gains from professional stretch therapy are cumulative and lasting, rather than the temporary improvements most people notice from occasional self-stretching.
The Dynamic Nature of Flexibility
One of the most consequential shifts in how leading practitioners and researchers understand flexibility is the move away from a static model toward a dynamic one. Flexibility is not a fixed property — it is a state that changes moment to moment in response to temperature, hydration, nervous system activation, movement history, and mechanical loading.
Practitioners and coaches in the high-performance space — including those working at the intersection of speed, power, and movement quality at facilities like the Parisi Speed School — have long recognized that the kind of flexibility that matters for athletic performance is not passive range of motion measured in a static stretch. It is the capacity to access and control range of motion under load, at speed, and in the dynamic patterns that sport and life actually demand.
This distinction has direct implications for how stretch therapy is designed and delivered. A session that only improves passive range of motion — how far a limb can be moved when the client is completely relaxed — addresses one dimension of flexibility. A session that also trains the nervous system to maintain access to that range of motion under active conditions addresses the dimension that actually transfers to performance, pain reduction, and functional daily movement.
"Flexibility without neuromuscular control is just a range your body can be moved into. Functional mobility is the range your body can move into, stabilize in, and return from — under the demands of real life."
This is the framework that informs how CNU Stretch practitioners are trained to work. The GYR (Green-Yellow-Red) feedback system is not just a safety tool — it is a real-time nervous system calibration protocol. By keeping clients in the Yellow zone — deep enough to be therapeutically productive, within the range the nervous system will accept — practitioners train both the tissue and the neurological permission that governs access to that tissue simultaneously.
Why Self-Stretching Has a Ceiling
Self-stretching is valuable. It is better than no movement. But it operates within significant constraints that most people never recognize — which is why consistent self-stretching rarely produces the mobility improvements people expect from it.
Why It Falls Short
- Cannot access deep fascial layers without external assistance
- Nervous system stays in protective mode — you cannot override your own stretch reflex
- No assessment — same stretches applied regardless of actual restriction pattern
- Targets symptoms, not fascial line sources
- No progressive overload protocol — same depth, same duration, same result
- No real-time feedback mechanism to calibrate depth
What Changes
- External assistance accesses fascial depth self-stretching cannot reach
- Practitioner works with the nervous system — not against it — using feedback and timing
- Assessment identifies the restriction source, not just the symptom site
- Fascial line approach addresses the origin of restrictions
- Progressive protocol tracks and advances range of motion over time
- GYR system provides real-time calibration of therapeutic depth
Peer-reviewed research on active-assisted stretching demonstrates that practitioner-guided techniques produce significantly greater range-of-motion improvements than passive or self-directed stretching — not because the techniques are dramatically different in appearance, but because the combination of external load, timing, nervous system engagement, and progressive protocol creates conditions for change that self-stretching simply cannot replicate.
What Professional Stretch Therapy Does Differently
Understanding the science of fascia and flexibility makes clear why professional stretch therapy produces results that self-stretching cannot. It is not that the stretches are more exotic. It is that the entire system — assessment, technique, nervous system engagement, feedback, and progression — operates on mechanisms that self-directed practice cannot access.
A certified stretch therapist using the CNU Stretch system works across all three layers of the flexibility problem simultaneously:
- Fascial tissue quality — using assisted and facilitated techniques to access adhesions and restrictions in the fascial layers that passive self-stretching cannot reach
- Fascial line assessment — identifying where in the connected chain a restriction originates, not just where it presents, and addressing the source
- Nervous system recalibration — using the GYR feedback framework and technique timing to progressively expand the range of motion the nervous system will permit without triggering defensive contraction
The result is not simply "feeling more flexible after a session." It is a cumulative, measurable expansion of functional range of motion — tracked over time using Kinotek AI movement analysis — that reflects genuine changes in both tissue quality and neurological permission. This is the difference between a session that feels good and a program that actually changes how a body moves.
Experience the Science in Practice
CNU Stretch practitioners are trained in fascial line assessment, neuromuscular re-education, and the GYR feedback system. Upcoming certification intensives in Delaware, Idaho, Virginia, and Oregon.
View Certification Dates